Adult Case Studies
Case Study #1
My first patient is41 y/o male who works as a CNA in a long-term
care rehab facility and as a cook in a restaurant. He injured his lower back
while helping a patient transfer from bed to w/c. His presented with severe
pain low back and sciatic pain with activity and at rest, antalgic gait with
lateral lean and pain that peripheralized to the mid posterior thigh at times.
Following his initial eval with the PT, she saw him two times and the PTA and I
saw him three times. On his first visit with the PTA and I, the patient
initially could not get into prone without 3 pillows under his pelvis. Initial
treatments included positioning for comfort, standing McKenzie wall extension,
wall side glides, manual therapy of lower paraspinals, piriformis and posterior
thigh, sciatic nerve glides, pelvic tilts and US. We also used a biofeedback
cuff while in supine to teach him to engage his TA and maintain the contraction
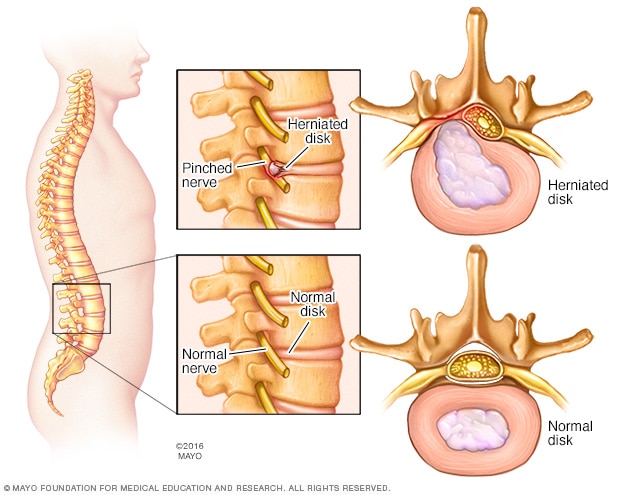
while breathing and marching. An MRI confirmed a herniated L4-L5 disc.
At the final session in which I was present before my clinical rotation ended, the patient was walking with improved gait and reported that his pain was reduced and centralized. It would still come into his glute area, but not all the time. The patient received lumbar traction in 90/90 supine for 10 minutes at 50% of his weight. He reported reduced pain after the treatment. Future interventions would include continued lumbar traction, core strengthening and education on proper lifting and transfer techniques.
This patient showed how as we age, our discs become less flexible and the amount of fluid in them is reduced which leads to greater risk of injury. Proper ergonomics and lifting techniques are important for preventing injuries like this.

Case Study #2
My second patient is a 46 y/o male who works as a general laborer in a local taconite mine. While hunting in Alaska he stepped in a hole and sustained a third-degree ankle sprain when he fractured his distal tibia, requiring ORIF with a plate and screws. When we started seeing him, he was back to work, and his job requires a great deal of walking. We did a lot of strengthening, stretching, joint mobes, kinesiotaping, MFR and STM, balance and proprioception activities. He was not yet at the stage for plyometrics by the time my clinical rotation ended. By his last appointment in which I was present, he walked with a normal gait pattern and his ROM had increased significantly. He had functional ROM of his ankle in all directions and was working toward full ROM. He still fatigued quickly, and his balance needed improvement, but he had made significant gains, stating that some days his pain and function were so good he would never know he had broken his ankle. Future interventions would include increasing strength, endurance, balance/proprioception and adding ballistic movements to return him to pre-injury functioning.
We also educated this patient on how important it was to challenge his balance and to provide neuromuscular reeducation because of the damage to his joints and how his proprioception was affected. If this isn't improved his chances of another injury are increased.
